Autism Spectrum Disorder (ASD) is a complex neurodevelopmental condition characterised by persistent challenges in social communication, restricted interests, and repetitive behaviours. Affecting individuals across all cultures and socioeconomic backgrounds, autism represents a broad spectrum of strengths and difficulties rather than a single uniform condition. Over the past two decades, rapid advances in genetics, neuroscience, digital health, and artificial intelligence have transformed scientific understanding of ASD and reshaped approaches to diagnosis and intervention. This article provides a comprehensive overview of autism, including its definition and epidemiology, underlying biological mechanisms, and the latest developments in diagnosis and treatment as of 2024–2026. Emphasis is placed on the multifactorial nature of ASD, the shift toward earlier and more precise detection, and the growing movement toward personalised and lifespan-oriented care.
Introduction to Autism Spectrum Disorder
Autism Spectrum Disorder (ASD) is defined as a neurodevelopmental condition that emerges early in life and persists across the lifespan. According to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), core features include difficulties in social interaction and communication, alongside restricted, repetitive patterns of behaviour, interests, or activities. The term“spectrum”reflects the wide variability in symptom presentation, cognitive ability, language skills, and support needs among autistic individuals.1
Globally, the prevalence of autism has risen steadily over the past two decades. In the United States, the Centers for Disease Control and Prevention (CDC) reported that approximately 1 in 31 children aged 8 years were identified with ASD in 2022, compared with 1 in 150 in the year 2000 (Figure 1). Similar trends have been observed in many other regions, largely attributed to increased awareness, broader diagnostic criteria, improved screening, and better access to services rather than a single environmental cause.2,3
Autism is not a disease in the traditional sense but a neurodevelopmental condition and a form of neurodiversity. Many autistic individuals view their traits as integral aspects of identity, emphasising the importance of respectful, strengths-based approaches to research and clinical practice.4 Nevertheless, significant challenges remain, particularly for individuals with co‑occurring intellectual disability, limited language, epilepsy, anxiety, or gastrointestinal problems, underscoring the need for continued scientific and clinical progress.4
Epidemiology and Clinical Features
ASD occurs in all racial, ethnic, and socioeconomic groups and is diagnosed more frequently in males than females, with a ratio of approximately 3–4:1. However, recent research suggests that autism in females and gender-diverse individuals may be underdiagnosed or diagnosed later in life due to different symptom profiles and compensatory behaviours such as social“masking”or "camouflaging".2,5,6,7
The core clinical features include:8
• Social communication differences: difficulties with reciprocal conversation, understanding nonverbal cues, and developing peer relationships.
• Restricted and repetitive behaviours: repetitive movements, insistence on sameness, intense interests, or sensory sensitivities.
• Developmental variability: language abilities range from fluent speech to minimal or absent verbal communication.
Many individuals with ASD also experience co‑occurring conditions, including attention‑deficit/hyperactivity disorder (ADHD), anxiety disorders, depression, sleep disturbances, and epilepsy. This clinical heterogeneity has been a major driver of contemporary research into mechanisms and personalised care.9
Biological and Neurodevelopmental Mechanisms of Autism
Genetic Architecture
Autism has a strong genetic basis, with heritability estimates ranging from 50% to 90% across studies. Modern genomic technologies, including whole‑exome and whole‑genome sequencing, have identified hundreds of genes associated with ASD risk. These include both rare, high‑impact mutations and common genetic variants that collectively contribute to polygenic risk.10
Current clinical genetic testing can identify a likely genetic cause in approximately 20–25% of individuals with ASD, particularly those with intellectual disability or syndromic features. Importantly, autism is not caused by a single“autism gene”but by the interaction of many genetic factors affecting early brain development.11
Brain Development and Neural Circuits
At the neurobiological level, ASD is associated with atypical brain development beginning during prenatal and early postnatal periods. Research has highlighted alterations in synapse formation, neuronal migration, and excitation–inhibition balance within cortical circuits.
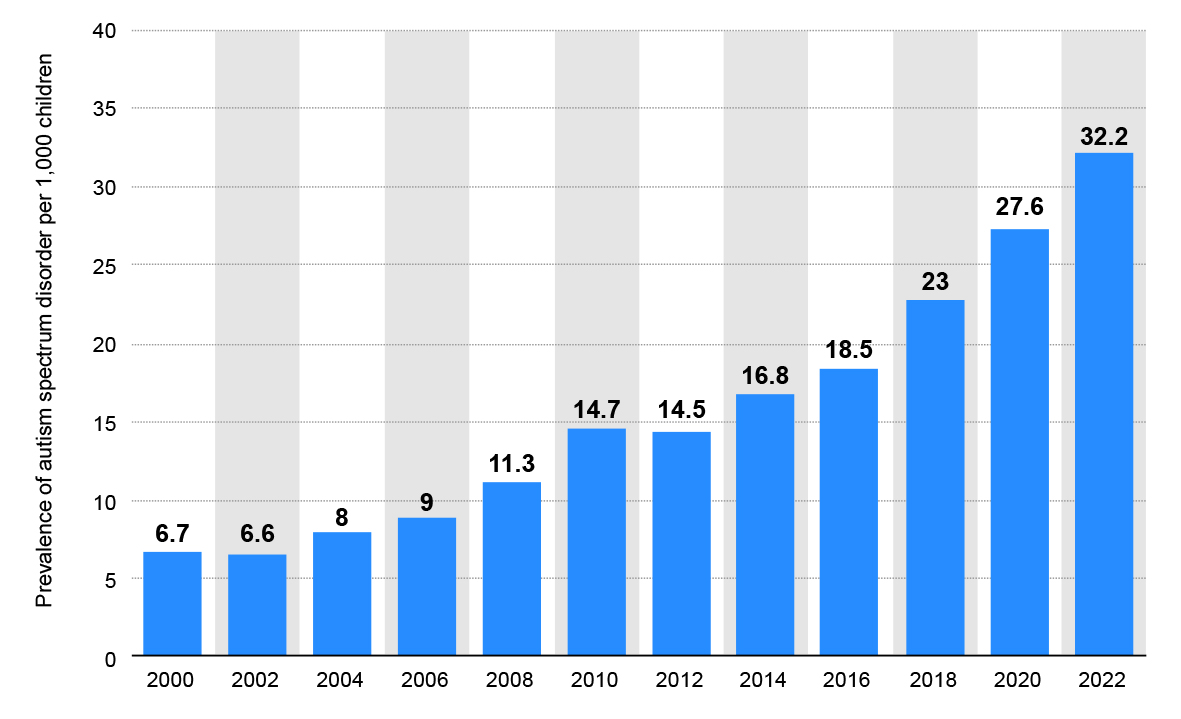
Figure 1. Prevalence of autism spectrum disorder in the U.S. from 2000 to 20222
These changes are thought to disrupt information processing relevant to social cognition, sensory integration, and behavioural regulation.9
Postmortem and neuroimaging studies have also identified differences in brain regions involved in social processing, such as the prefrontal cortex, temporal lobes, amygdala, and cerebellum, although findings vary across individuals.12
Molecular Pathways and Neuroinflammation
Converging evidence suggests that multiple molecular pathways contribute to ASD, including those involved in synaptic signalling, transcriptional regulation, and immune function. Dysregulation of inflammatory and immune-related genes has been observed in both blood and brain tissue from autistic individuals, supporting a role for neuroinflammation in at least a subgroup of cases.11,13
The Gut–Brain Axis
An emerging area of research focuses on the gut–brain axis. Many autistic individuals experience gastrointestinal symptoms, and studies have reported altered gut microbiota composition and increased intestinal permeability in subsets of ASD. These changes may influence brain development and behaviour through immune, metabolic, and neurotransmitter-related pathways, although causality remains under investigation.14
Advances in Autism Diagnosis
Traditional Diagnostic Approaches
Currently, autism diagnosis relies on comprehensive clinical evaluation, including developmental history, direct behavioural observation, and standardised instruments such as the Autism Diagnostic Observation Schedule (ADOS) and Autism Diagnostic Interview–Revised (ADI‑R). While these methods are effective, they are time‑consuming, require specialised expertise, and may contribute to delays in diagnosis.15
Early Screening and Digital Tools
Routine developmental screening at 18 and 24 months is widely recommended, enabling diagnosis as early as 18 months in some children. Recent years have seen rapid growth in digital health tools designed to support earlier and more accessible screening.16
The gaze patterns of individuals with autism can significantly diverge from those of neurotypical individuals. For instance, many autistic individuals might engage in prolonged staring or avoid direct eye contact, behaviours that can be misinterpreted by others as rudeness or disinterest.17 Artificial intelligence (AI) and machine‑learning approaches using eye‑tracking, facial analysis, voice patterns, and video-based behavioural data have shown promising accuracy in distinguishing autistic from typically developing children. A 2026 systematic review reported pooled diagnostic accuracy of approximately 85% for machine‑learning models based on eye‑tracking data, highlighting their potential as objective screening aids.18,19
Genetics and Biomarkers
Genetic testing is increasingly incorporated into the diagnostic workup, providing etiological insights and informing medical management. However, despite intensive research, no validated biological biomarkers are currently available for routine autism diagnosis, and experts caution against premature clinical adoption of experimental markers.11,15
Current and Emerging Treatments for Autism
Behavioural and Developmental Interventions
Evidence-based behavioural and developmental interventions remain the cornerstone of autism care. Approaches such as Applied Behaviour Analysis (ABA), naturalistic developmental behavioural interventions, speech and language therapy, and occupational therapy have demonstrated benefits in communication, adaptive functioning, and quality of life, particularly when initiated early.20
Pharmacological Management
At present, no medication treats the core features of autism. Pharmacotherapy is primarily used to manage co‑occurring symptoms such as irritability, aggression, anxiety, ADHD, and sleep disturbances. Recent FDA approval of trofinetide for Rett syndrome—a genetic condition with autistic features—highlights progress in targeted treatments for specific subtypes.9, 11
Precision Medicine and Gene‑Targeted Therapies
One of the most significant recent shifts in autism research is towards precision medicine. Advances in genomics, brain organoids, and molecular neuroscience are enabling the development of gene‑specific and pathway‑targeted therapies, particularly for rare monogenic forms of ASD. While these approaches are largely experimental, they represent a major step toward individualised treatment strategies.11,21
Microbiome‑Based and Novel Interventions
Interventions targeting the gut microbiome—such as probiotics, dietary modifications, and faecal microbiota transplantation—have shown preliminary promise for improving gastrointestinal and, in some cases, behavioural symptoms. However, clinical evidence remains limited, and large, controlled trials are needed before widespread clinical adoption.14
ASD Care Coordination
Because of the complexity of autism, the assessment and management should be done with the help of a multidisciplinary team, which consists of a developmental paediatrician, psychiatrist, psychologist, audiologist, occupational therapist, speech therapist, special educator, and social worker (Figure 2).22
The expanding practice of multidisciplinary care to address the complex nature of ASD suggests that there is a need for a means of coordinating care that transcends the disciplinary distinctions of relevant ASD treatment providers. As ASD services become more specialised, there is a growing need for effective care coordination with providers across the systems of care.23
Autism care coordination involves organising services across health, education, and community sectors to support individuals with ASD. It focuses on creating a personalised, family-centred plan to improve quality of life, streamline access to specialists (e.g., occupational therapy and speech therapy), and reduce caregiver stress.24
The core components of autism care coordination include: 24
• Family-Centred Approach: Focuses on family priorities, strengthening partnerships between parents and providers.
• Individualised Planning: Creating a comprehensive plan that acts as a roadmap, addressing unique medical, educational, and social needs.
• Centralised Communication: Ensuring all providers (specialists, schools, therapists) are aligned on the same goals.
• Transition Support: Assisting with transitions, particularly from early intervention to school, or from paediatric to adult care.
• Resource Navigation: Identifying and accessing community resources, financial assistance, and, if necessary, Special Child Care Institutions.
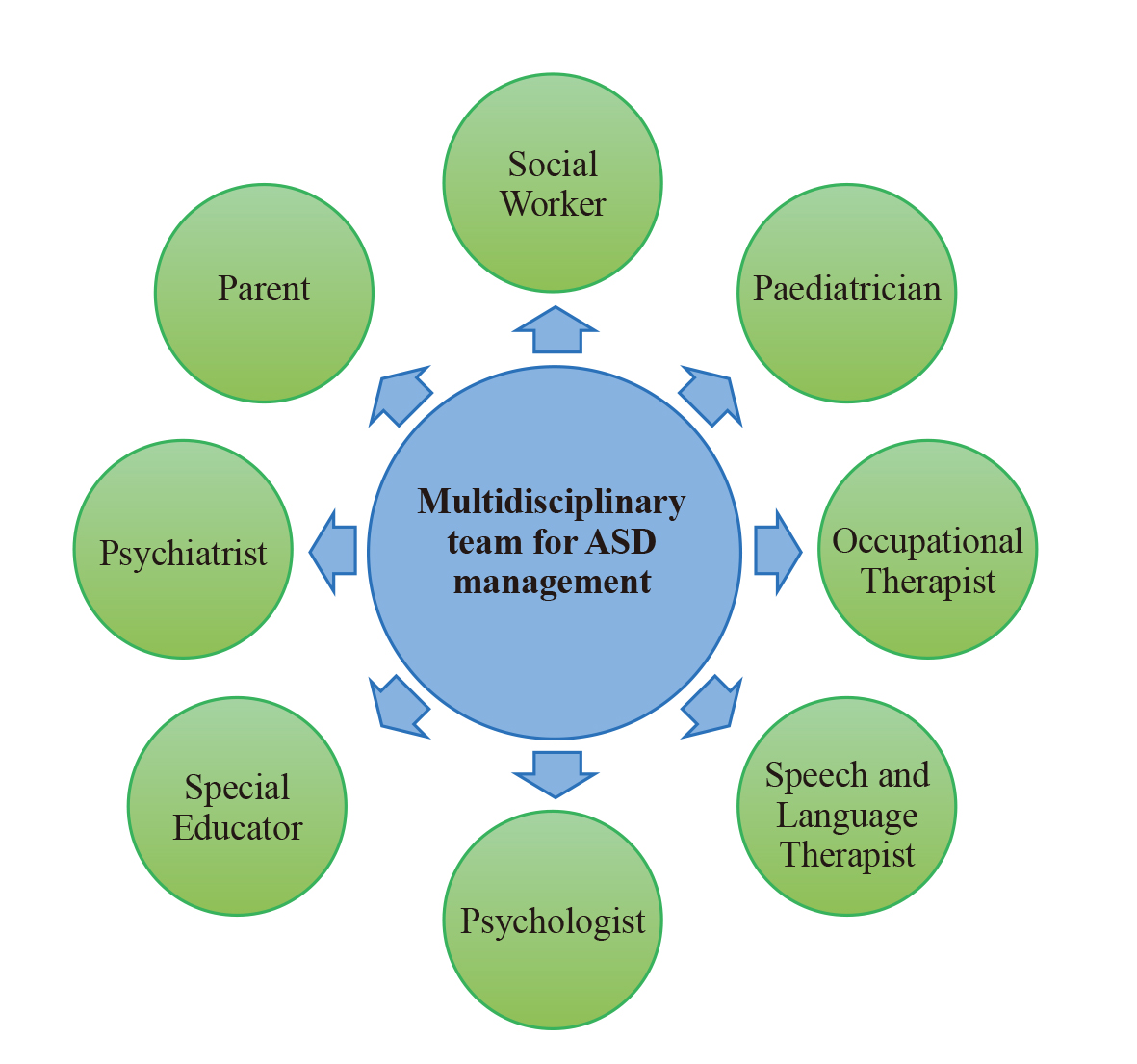
Figure 2. Multidisciplinary approach managing autism spectrum disorder22
ASD care coordination offers profound benefits for families and providers alike. By streamlining communication among healthcare professionals, therapists, and educators, coordination significantly reduces stress for families who would otherwise face the overwhelming task of navigating complex care systems on their own. This relief allows parents to focus more on supporting their child rather than managing fragmented services. It also drives improved outcomes, ensuring that children receive timely access to therapies and interventions. With a coordinated approach, care plans are more consistent, progress is monitored effectively, and children are less likely to experience delays in receiving essential support. Furthermore, care coordination strengthens continuity of care, preventing gaps in services that can disrupt a child's development. By maintaining a steady flow of communication and planning across providers, children benefit from stable, long-term support that adapts to their evolving needs. In essence, ASD care coordination is not just about logistics—it is about creating a smoother, more reliable path toward growth and well-being for both children and their families.23
Ethical Considerations and Future Directions
As scientific understanding of autism advances, ethical considerations are increasingly central. Autistic self‑advocates emphasise the importance of research that respects neurodiversity, avoids stigmatisation, and prioritises quality of life and autonomy. Future research directions include improved support across the lifespan, better services for adults and aging populations, and greater inclusion of under-represented groups in studies.5
Large international collaborations and multimodal datasets are expected to accelerate discovery of clinically useful biomarkers, refine subtyping, and enhance translation from laboratory findings to real‑world care.15
Conclusion
Autism Spectrum Disorder is a highly heterogeneous neurodevelopmental condition shaped by complex interactions among genetic, biological, and environmental factors. Over the past decade, and particularly from 2024 onwards, remarkable progress has been made in elucidating its mechanisms, improving diagnostic practices, and developing more personalised interventions. While no cure exists, early identification, evidence‑based support, and emerging precision medicine approaches offer growing opportunities to enhance outcomes and quality of life for autistic individuals and their families. Continued interdisciplinary research, ethical engagement, and inclusive policy development will be essential as the field moves forward.
References
1. Cortese S, et al. Cell Rep Med. 2025;6(2):101916. 2. CDC. Data and Statistics on Autism Spectrum Disorder. 27 May 2025. Available from:
https://www.cdc.gov/autism/data-research/index.html. [Accessed 2 April 2026]. 3. Kumar A and Bhattacharya S. Front Child Adolesc Psychiatry. 2024;3:1489269. 4. Urbanowicz A, et al. Autism Adulthood. 2019;1(2):82-9. 5. Autism Speaks. Research roundup: 2024 in review and the road ahead. 18 December 2024. Available from: https://www.autismspeaks.org/science-news/autism-research-2024. [Accessed 2 April 2026]. 6. Gellert B, et al. Behav Sci (Basel). 2025;15(8):1073. 7. Adult Autism Health Resources, Harvard Medical School. How is Autism Di[erent in Women? Available from: https://www.adult-autism.health.harvard.edu/resources/how-is-autism-di[erent-infemales/.[Accessed 2 April 2026]. 8. Hodis B, et al. Autism Spectrum Disorder. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK525976/. [Accessed 2 April 2026]. 9. Lamanna J and Meldolesi J. Int J Mol Sci. 2024;25(4):2423. 10. Eyring KW and Geschwind DH. Hum Mol Genet. 2021;30(20):R236-R244. 11. Autism Science Foundation. 2024 Autism Science Review. Available from: https://autismsciencefoundation.org/year-end-summary-2024/. [Accessed 2 April 2026]. 12. Holanda MVF, et al. Front Psychol. 2025;16:1558081. 13. Jiang CC, et al. Signal Transduct Target Ther. 2022;7(1):229. 14. Hetta HF, et al. Mol Neurobiol. 2025;63(1):211. 15. Cortese S, et al. Cell Rep Med. 2025;6(2):101916. 16. Hyman SL, et al. Pediatrics. 2020;145(1):e20193447. 17. Alsharif N, et al. Front Med (Lausanne). 2024;11:1436646. 18. Ahmed M, et al. Appl Sci. 2025; 15(14): 8056. 19. Han W, et al. Int J Med Inform. 2026;208:106235. 20. Qin L, et al. Eur J Med Res. 2024;29(1):322. 21. Hong D and Iakoucheva LM. Transl Psychiatry. 2023;13(1):58. 22. Uke P, et al. Cureus. 2024;16(6):e62753. 23. Parker ML, et al. Issues Ment Health Nurs. 2020;41(2):138-45. 24. McClain MB, et al. Interprofessional care coordination for pediatric autism spectrum disorder: Translating research into practice. Springer International Publishing, 2020.